VASCULAR CONDITION
Varicose Veins Treatment
Varicose veins are enlarged, dilated veins that commonly affect the thigh, legs. It causes pain, swelling, and skin changes like discolouration and itching. They develop due to weakened vein valves that disrupt normal blood flow.
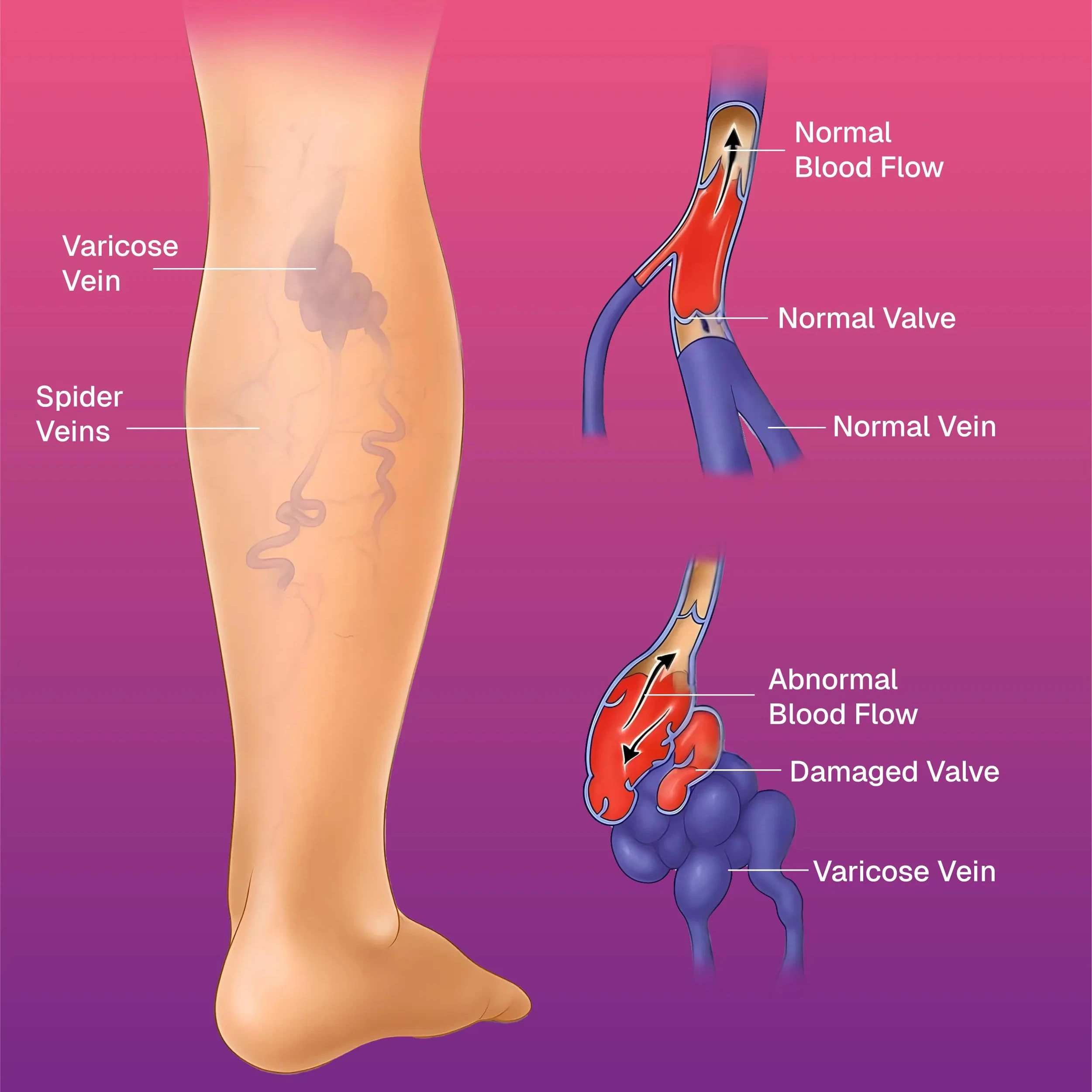
What Are Varicose Veins?
Varicose veins are enlarged, twisted veins that develop when the valves inside the veins become weak or damaged. These valves normally ensure one-way blood flow toward the heart. When they fail, blood pools in the veins, causing them to stretch and become visible under the skin.
They most commonly affect the legs due to increased pressure from standing and walking. While varicose veins are often considered a cosmetic concern, they can also lead to discomfort, swelling, skin changes, itching and, in advanced cases, complications such as ulcers or bleeding.
There are six stages from early spider veins to advance discoloration and ulcer.
Common Symptoms
• Visible, bulging veins on the legs
• Aching, heaviness, or discomfort after standing
• Swelling around the ankles or calves
• Itching or skin irritation near affected veins
• Skin discoloration or thickening around the ankles
• Non-healing ulcers in advanced cases
When to See a Doctor
• Persistent leg pain, swelling, or heaviness
• Skin color changes or hardening near the ankle
• Bleeding from varicose veins
• Development of open sores or ulcers
• Sudden leg swelling or pain (to rule out blood clots)
Causes and Risk Factors
Varicose veins develop when increased pressure and weakened vein valves interfere with normal blood flow in the legs. Several factors can increase the likelihood of developing this condition.
• Family history of venous disease
• Prolonged standing or sitting
• Advancing age
• Pregnancy and hormonal changes
• Obesity
• Previous blood clots or vein injury
Diagnosis and Evaluation
Diagnosis of varicose veins begins with a detailed clinical assessment, including a review of symptoms and physical examination of the affected limbs. The goal is to understand the severity of vein involvement and identify any underlying circulation issues.
A Doppler ultrasound examination is commonly used to evaluate blood flow within the veins, assess valve function, and detect reflux or obstruction. Additional imaging studies may be recommended in selected cases to guide treatment planning.
Evaluation may include:
• Clinical examination
• Doppler ultrasound imaging
• Assessment of venous reflux and obstruction
Treatment Options
Treatment for varicose veins depends on the severity of symptoms, extent of vein involvement, and overall health of the patient. Management is individualized, with a preference for minimally invasive approaches whenever appropriate.
• Lifestyle modification and compression therapy
• Minimally invasive endovenous procedures
• Endovenous laser treatment (EVLT), where appropriate
• Sclerotherapy for suitable veins
• Image-guided interventions for advanced disease
Diagnosis of varicose veins begins with a detailed clinical assessment, including a review of symptoms and physical examination of the affected limbs. The goal is to understand the severity of vein involvement and identify any underlying circulation issues.
A Doppler ultrasound examination is commonly used to evaluate blood flow within the veins, assess valve function, and detect reflux or obstruction. Additional imaging studies may be recommended in selected cases to guide treatment planning.
The choice of treatment is determined after clinical evaluation and imaging, with the goal of relieving symptoms, improving circulation, and preventing complications.
Its a DAY CARE procedure and you can go to your daily activity on very same day or next day .!
Role of Interventional Radiology
Interventional radiology plays a key role in the management of vascular conditions by using image-guided, minimally invasive techniques to diagnose and treat disease. These procedures are performed through small access points, allowing precise treatment while minimizing damage to surrounding tissues.
Compared to traditional open surgery, interventional radiology procedures often involve less pain, lower risk of complications, and shorter recovery times. Treatment decisions are based on clinical evaluation and imaging findings, with a focus on safety, effectiveness, and long-term outcomes.
Frequently Asked Questions
Are varicose veins a serious condition?
Varicose veins are often not life-threatening, but they can cause discomfort and may lead to complications such as skin changes, ulcers, or bleeding if left untreated.
Is surgery always required for varicose veins?
Surgery is not always required. Many cases can be managed with minimally invasive, image-guided procedures depending on the severity of symptoms and vein involvement.
Are minimally invasive treatments painful?
Most minimally invasive treatments are well tolerated and performed with local anesthesia. Discomfort is usually minimal compared to traditional surgical approaches.
How long does recovery take after treatment?
Recovery time varies depending on the procedure performed. Many patients are able to resume normal activities shortly after minimally invasive treatment, as advised by their doctor.
Can varicose veins come back after treatment?
Treated veins usually do not recur, but new varicose veins may develop over time. Regular follow-up and lifestyle measures can help reduce recurrence.
